This is the second article in a three-part series about changes at McDonough District Hospital during its 67 years that have affected and improved its services.
Healthcare is one of the most-regulated industries in the country, and hospitals must meet local, state and federal mandates to keep their doors open and receive payment for services. Besides these regulations, hospitals set their own rules, such as visiting hours. At least one rule change at McDonough District Hospital was driven by patients.
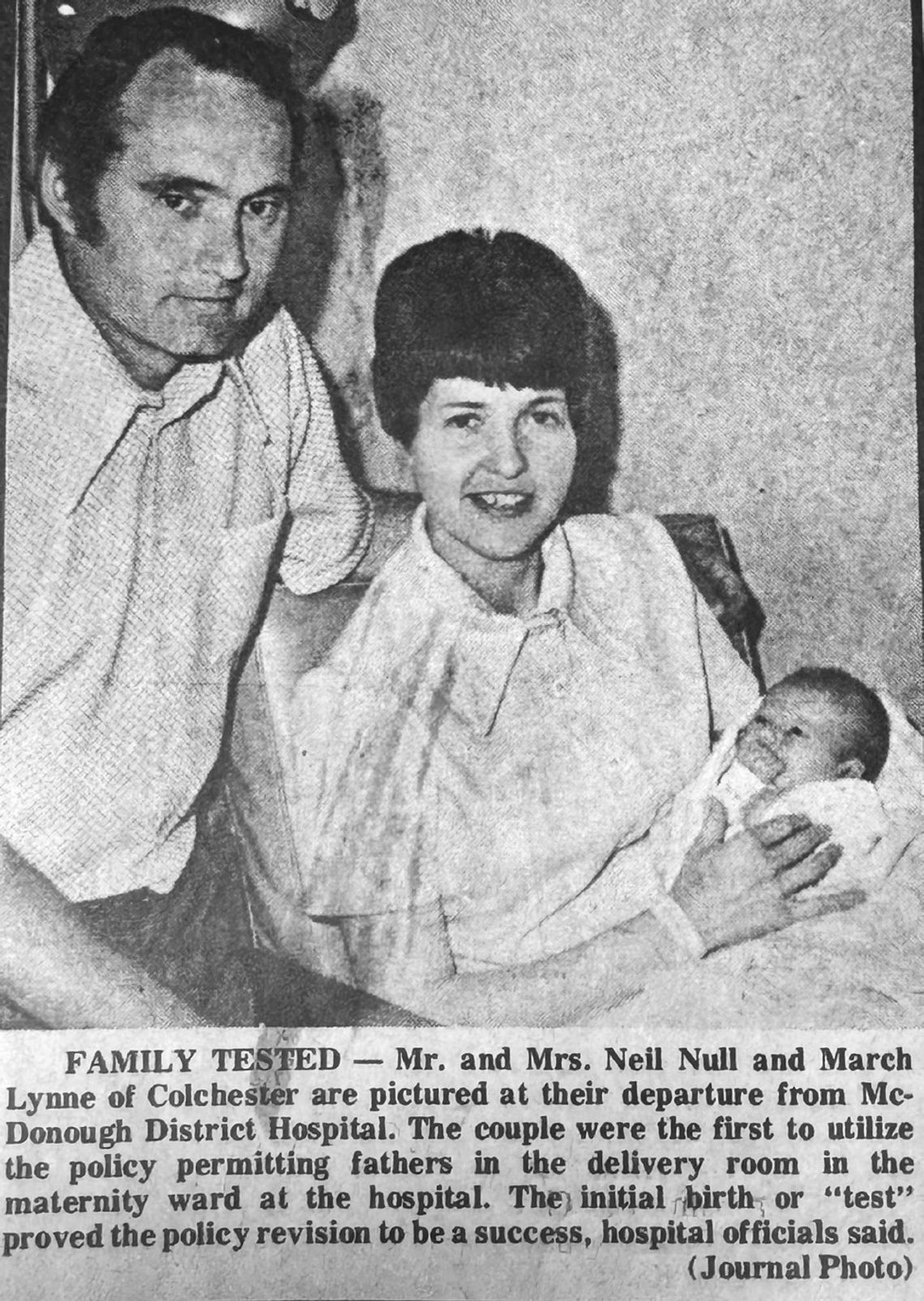
Having fathers in the delivery room is so commonplace now that people may be unaware that fathers weren’t allowed in delivery rooms at MDH until 1974 – only after they had completed a prenatal course sponsored by the hospital. The change came after women began leaving the community to have their babies.
According to an article published in the Macomb Daily Journal in early 1974, the number of births at MDH began declining after hospitals in Carthage, Canton and Galesburg, and Keokuk, Iowa, started allowing fathers in the delivery room.
The first mother-father delivery duo was Neil and Linetta Null, whose daughter Marcy Lynne was born on June 8, 1974.
Earning accreditations and certifications Patient satisfaction and quality in the hospital’s obstetrics unit has continued for more than 50 years. In its most-recent recognition, MDH received the 2025 Illinois Birthing Hospital Quality Excellence Award from the Illinois Perinatal Quality Collaborative. The designation came with a $20,000 award to support enhanced quality-improvement and equity initiatives within the hospital’s obstetrics services.
The most-important accreditation for MDH is earning Joint Commission’s seal of approval because it is required to receive payments from Medicare and Medicaid. Although there are other accreditation agencies, Joint Commission sets the gold standard for measuring healthcare quality and patient safety.
MDH has been accredited by Joint Commission since 1960. The hospital received a score equivalent to 99 percent on its 2023 survey. The next survey will be in 2026.
“One of the surveyors commented, ‘I see a survey with this positive level of quality about once every five years’,” said Wanda Foster, who oversaw survey preparation. The former vice president of nursing retired in early 2025 after working at the hospital for nearly 44 years. Now she serves on the MDH Board of Directors. “We had the perfect synergy of our clinical directors and ancillary directors and entire MDH team working in sync to attain these excellent findings. It’s a remarkable achievement for the organization.”
Foster said hospitals nationwide have increased their focus on quality and safety in the last 10 years. She said MDH’s best reflection of this is its continued “A” ratings in voluntary surveys by The Leapfrog Group, an independent national nonprofit watchdog focused on patient safety. The organization gives hospitals letter grades based on more than 30 measures of errors, accidents, injuries and infections as well as systems hospitals have in place to prevent them.
MDH is one of 35 hospitals in Illinois to receive an “A” grade for fall 2025.
MDH also holds these accreditations and designations: • Acute Stroke Ready Hospital – Illinois Department of Public Health
• Cardiac Rehabilitation – American Association of Cardiovascular and Pulmonary Rehabilitation
• Cardiovascular Laboratory – Joint Commission
• Diabetes Education Center – American Diabetes Association
• Home Health and Hospice – Joint Commission
• Medical Laboratory – College of American Pathologists
• Radiology (mammography) – American College of Radiology
• Sleep Laboratory – Joint Commission Following government regulations Two governmental acts in the late 1990s and early 2000s have greatly affected the way the hospital handles patient information: the Health Insurance Portability and Accountability Act (HIPAA) and the Health Information Technology for Economic and Clinical Health (HITECH) Act of 2009.
Publishing patient admissions, dismissals and births in the Macomb Daily Journal began when the hospital opened and continued until the late 1980s or early 1990s. Although that is unimaginable today, providing this patient information was a practice of many hospitals. It ended at MDH many years before the enactment of HIPAA’s 2003 privacy rule, which gives patients the right to authorize how their personal health information can be shared beyond essential hospital operations. The HITECH Act gave healthcare organizations about five years to implement electronic medical records (EMRs) before penalties would be issued.

MDH met the deadline. The use of an EMR led to the introduction of the hospital’s online patient portal in 2019. On the portal, patients who are 18 or older can access information such as clinic visit summaries, medications, allergies, procedures and test results.
Tying the two mandates together, HIPAA gives patients the right to obtain an electronic copy of their medical records.
Compensating a large workforce Paying employee wages has always been a large part of any hospital’s budget.
MDH’s 2025 financial report showed the total cost of employee wages and benefits for its nearly 500 employees, which includes physicians, was $50.2 million of the year’s operating revenue of $84.7 million.
In 1966, the starting pay for a registered nurse at MDH was $475 a month.
That pay was increased to $499 per month after four or five years of service. In 1980, the registered nurse salary range was $7 to $9.89 per hour. At that time, the minimum wage in Illinois and the U.S. was $2.30 per hour.
In a recent search of job openings at the hospital, the pay range for a registered nurse in the Obstetrics Unit is $34 to $54.40 per hour.
Wage scales for other open positions are:
• Athletic trainer, $22.76 to $34.14
• Certified occupational therapist assistant-Home Health, $24.36 to $36.53
• Environmental Services aid, $15 to $20.25
• Medical assistant, Bushnell Clinic, $18.58 to $26.02
• Patient Access specialist, clinic, $17.55 to $23.69
• Nuclear medicine technologist, $37.59 to $56.38
• X-ray technologist $24.36 to $36.53 Paying the price for health care Medicare and Medicaid didn’t exist when MDH opened. The bill creating these government-paid resources was signed into law by President Lyndon Johnson in 1965. Until then, patients relied on commercial insurance or paid the entire bills themselves.
Now, about 50 percent of MDH patients are enrolled in Medicare and 20 percent are enrolled in Medicaid.
Other patients have commercial healthcare insurance, such as Blue Cross Blue Shield and Aetna, and some have no insurance.
Payments to the hospital from the three types of insurance groups are based on a complicated web of rules including rates for negotiated fees and, in some instances, higher payments for better outcomes. For the 70 percent of MDH patients enrolled in government programs, MDH receives about 50 percent reimbursement for the cost of providing care to these patients.
The reimbursement rate for commercial insurance payers is higher, but not 100 percent.
“One of the big challenges is just getting paid,” said MDH President and CEO Bill Murdock. “You’re constantly chasing down the insurance companies, fighting denials, fighting rejections. Getting paid what you deserve is a challenge.”
For patients who don’t have insurance, a billing category called “self-pay,” paying 100 percent of a hospital bill is likely impossible. They may be eligible to receive a 40 percent discount on their care through the hospital’s financial assistance program. As a not-for-profit hospital, MDH has a charitable mission to provide care to patients who cannot afford to pay. Last year, it provided more than $5 million in care for which no payment was received.
Finding funding from other sources The “district” in MDH’s name stems from its origins of being supported by taxpayers in McDonough County – the district. In 1973, 12.3% percent of all sources of funds for the hospital came from taxpayers.
In 1982, 4.1% of funds were from taxpayers. In the mid-1980s, MDH voluntarily eliminated the property tax subsidy, and began relying on its own earnings to support operations. At the time, MDH also assumed financial responsibility for the ambulance service, which had been subsidized by McDonough County.
An ongoing source of funding began in 1973 when MDH became the largest beneficiary of Lulu Fellheimer’s estate. The nearly $3.7 million gift was in the form of a trust to be used for care for the elderly and people lacking financial means to otherwise receive such care, health career scholarships and physician recruitment.
More recently, after Dick Switzer’s wife died in 2013, he donated $1.9 to MDH to be seed money for the future Dolores Kator Switzer Women’s Center. The $8 million center featuring a new obstetrics unit, remodeled mammography areas, and ultrasound and bone density suites, opened in 2020. When Switzer died in 2016, he left his estate to the hospital, creating a total gift of $2.6 million.
In 1996, MDH Board of Directors established the MDH Development Council to provide financial support for the hospital. At that time, it also started a group of employee donors named PROS – Professionals Reaching Out in Support.
“When employees are out supporting the organization for which they work, that emphasizes their commitment and boosts the hospital’s integrity,” Foster said.
The council evolved into the McDonough District Hospital Foundation, a charitable organization with a board of directors. It helps fund projects that improve patient care, enhance staff training and support community health. Current initiatives include funding a new mammography system, endoscopy scopes and SimMan, a realistic patient simulator that breathes, bleeds, sweats, blinks and talks through a microphone system. The high-tech training device enables hands-on learning for staff.
“The foundation is very vital for us when we’re looking to purchase new equipment or a new service, or if staff need help with some education,” Murdock said. “The foundation’s been a great resource for us. They provide the funds that we need to meet our goals.”
The foundation raises money through special events, such as the annual golf tournament and other special events, one-time gifts, pledges, memorials, endowments and gifts of grain. According to the MDH website, “Income from gifted grain is not recognized on your tax return, meaning it is never reported as income. This can reduce your adjusted gross income and result in savings on income and self-employment taxes.”
The MDH Auxiliary, which had raised money for the hospital, now uses money from its Gift Gallery on the hospital’s first floor to provide $15,000 to $20,000 in scholarships each year.
Read Friday's edition of the Community News Brief for Part three of this series which will focus on the hospital’s efforts to ensure its future in Macomb.